
Worldwide, more than 15 million babies are born prematurely each year. In the US, that number is close to 500,000. Due to the increased incidence of multiple births resulting from fertility treatments, as well as medical technology that has increased the survival rates for extremely preterm babies, the numbers are rising. Between 5% and 18% of babies worldwide are born prematurely.
Premature babies are classified according to gestational age. The average pregnancy lasts 40 weeks. Babies who arrive at between 37 weeks are considered ‘moderate to late’ preemies; ‘very preterm’ at 28-32 weeks; and ‘extremely preterm’ at 28 weeks or less. Babies who weigh less than 1 3/4 pounds, or are born at 26 weeks or less, are often referred to as ‘micro preemies.’
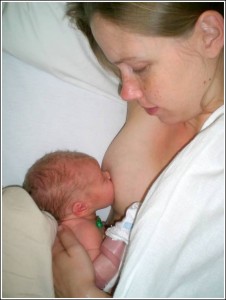
While all newborn babies receive many nutritional, immunological, physiological, and neurological benefits from breast milk, the advantages to premature babies are even more important.
Every mother produces breast milk that changes to meet the needs of her baby at different stages of life. Milk produced by the mother of a toddler has a different composition from the milk produced for a newborn, and milk from a mother who has given birth prematurely is different from that produced for full term babies.
Breast milk produced by the mother of a preemie has extra nutrients (calories, fat, protein, and vitamins) to help these tiny babies grow quickly. It contains live cells and antibodies to protect their immature immune systems from infections, and is easier for preemies to digest than formula.
Premature babies are often too immature to feed at the breast immediately after birth. In addition to prematurity, they often have medical problems, and may be placed in the NICU (Neonatal Intensive Care Unit) until they are stable enough to feed successfully via bottle or breast. ‘Non-nutritive sucking’ (NNS) involves letting the preemie nurse from the mothers breast, which is emptied by pumping before the feeding. A pacifier is offered at the same time, which stimulates breast milk production. The baby tastes and licks the breast while sucking the pacifier, which provides oral stimulation that a breast pump can’t. Preemies have a lot of catching up to do, and breastfeeding helps speed up the process.
Since preemies are often separated from their mothers for long periods of time, it’s important to begin stimulating the breasts as soon after birth as possible by using an effective double breast pump. The hospital lactation consultant is an important member of the preterm baby’s medical team. She will help the mother locate a hospital grade pump, give instructions on how to use it, and provide information on how often to pump and how to store her breast milk. Insurance often covers the cost of hospital grade pumps when medically necessary.
The lactation consultant will work closely with the mother and baby in making the transition to feedings at the breast. She may recommend the use of a nipple shield to increase milk transfer, or suggest a prescription medication like Domperidone or Reglan to increase milk supply if needed. Weight checks and milk intake monitoring to make sure the baby is getting enough milk, and to help measure his progress.
Immediately after birth, the breasts produce colostrum – a fluid so rich in antibodies that it’s often called the baby’s ‘first vaccine’. Colostrum is only present in breast milk for the first week or so after birth, so it’s especially beneficial for the mom to pump often during that time. Because preemies are smaller than full term babies, they take less milk per feeding. When it comes to breast milk – and especially colostrum – every drop counts!
Preemies too immature to feed at the breast can still receive mama’s milk via tube feeding or a (NG) tube (known as gavage). It may take some time before they are able to move from tube feeding to breast or bottle, because they have difficult coordinating their sucking and swallowing. During early feedings at the breast, many babies aren’t able to latch on and suck effectively.
Since preemies are often in the NICU for extended periods of time, they don’t get the same skin-to-skin contact as full term babies who aren’t separated from their mothers. One way to provide this closeness and touch is ‘kangaroo care’.
Kangaroo care involves holding the baby as much as possible, and both mothers and fathers can offer this skin-to-skin contact. Due to the many benefits of kangaroo care (increased bonding, easier transition to breastfeeding, more coordinated breathing, lower blood pressure, reducing the pain of heel sticks, and better sleep patterns), most hospitals will offer some version of kangaroo care. Researchers have also found evidence that when parents speak to their preemies, there is an improvement in their baby’s language scores when they begin to talk. Discuss the importance of early interaction and skin-go-skin contact with your health care provider. .
 Preemie moms are under a great deal of stress, and not surprisingly, are more prone to depression than the mothers of full term babies. They aren’t able to build their milk supply by getting breast stimulation from a healthy full term baby, so they have to spend time hooked up to a machine, and even the most expensive breast pumps not as effective as a baby nursing directly at the breast.
Preemie moms are under a great deal of stress, and not surprisingly, are more prone to depression than the mothers of full term babies. They aren’t able to build their milk supply by getting breast stimulation from a healthy full term baby, so they have to spend time hooked up to a machine, and even the most expensive breast pumps not as effective as a baby nursing directly at the breast.
Instead of being at home resting with their nursling nestled in their arms, preemie moms are traveling back and forth to the NICU, which is a scary and intimidating place. Fragile little babies spend most of their time in plastic boxes, surrounded by beeping machines and bright lights, connected to tubes, and cared for by multiple medical experts. The NICU is the last place any parent wants to be, and they can’t wait to take their baby home. Studies show that breast fed babies spend less time in the hospital than formula fed babies, which is another advantage of breastfeeding.
All this occurs at a time when moms are hormonal, recovering from childbirth, and dealing with sleep deprivation. Mothers of premature babies need to remember to take care of themselves, although that’s hard to do because they are so consumed with worry about their babies. It’s important to develop a ‘safety net’ of support from family, friends, or support groups like La Leche League to help new moms cope with the challenges faced by the arrival of a sick or premature infant. Finding a support group of other preemie moms is also helpful. There are lots of support groups on Facebook.
Most mothers who give birth prematurely are able to produce just as much milk as mothers of full term babies. Those who aren’t able to produce enough milk for whatever reason may be able to obtain breast milk from a human milk bank. Milk banks carefully screen donors who provide breast milk for these tiny and vulnerable preemies. Due to the proven multiple advantages of breastfeeding, doctors can prescribe donor milk for preemies because it’s considered ‘medically necessary’. Insurance often pays for donor milk.
Mothers who are actively involved in their premature baby’s care by providing him with the benefits of breastfeeding are giving him a priceless gift that only she can give!
Here are some helpful resources for preemie moms:
This NICU glossary includes medical terms mothers will hear during their baby’s hospital stay:
http://www.preemiebabies101.com/nicu-staff/
Preemie babies 101 has good general information about prematurity:
http://www.preemiebabies101.com/
Here’s a blog post about one mom’s experience in the NICU:
“Two days after I hit 28 weeks, I delivered my baby girl. She made it the 48 hours the doctor and I were hoping and praying for, so that the steroid shot could develop her lungs, and then my perfect, boring pregnancy was over in exactly two drugged up pushes. She weighed 2 pounds, 10 ounces, and looked a lot like a baby bird who had fallen out of the nest too soon, which is kinda what happened, if you think about it.”
http://www.breastfeedingbasics.com/muffins-minion/nicu-1-dont-bomb-anyone Anne Smith, IBCLC
Anne Smith, IBCLC
Breastfeeding Basics
 Breastfeeding Basics
Breastfeeding Basics




