 The art of breastfeeding in something that you learn by doing, and it gets easier with practice. In the old days, young women grew up seeing their family members and friends nurse. Breastfeeding was the norm, unlike today where we live in a bottle feeding culture. In today’s society, many women have never seen anyone nurse a baby. The idea of taking classes or reading books to learn about breastfeeding would have made our great grandmothers laugh, but in today’s world, it makes sense to learn as much as you can about breastfeeding before your baby is born.
The art of breastfeeding in something that you learn by doing, and it gets easier with practice. In the old days, young women grew up seeing their family members and friends nurse. Breastfeeding was the norm, unlike today where we live in a bottle feeding culture. In today’s society, many women have never seen anyone nurse a baby. The idea of taking classes or reading books to learn about breastfeeding would have made our great grandmothers laugh, but in today’s world, it makes sense to learn as much as you can about breastfeeding before your baby is born.
If possible, attend a prenatal breastfeeding class. Many hospitals, doctor’s offices, and health departments offer them at no charge, or for a small fee. If there is a group in your area, attend La Leche League meetings during your pregnancy. La Leche League is the original breastfeed support group, and has been going strong for nearly sixty years. It’s still the world’s largest source of breastfeeding support and information, and has well trained volunteers – all women who have breastfeed at least one baby for at least a year – who provide free mother to mother support all over the world.
There are many books about breastfeeding on the market, and some are better than others. If you only buy one resource book, The Womanly Art of Breastfeeding is by far the best, even if it does have a cheesy name. It not only contains detailed information about all aspects of nursing your baby, but also goes into detail about nutrition, starting solids, attachment parenting, and weaning. This is a book that you will refer to over and over again, not just during the early days of breastfeeding.
One thing is for sure: childbirth and breastfeeding are two experiences that no amount of reading, attending classes, joining Facebook groups, or watching videos can really prepare you for. What they mostly do is tell you about what the average’ birth experience or the “average” breastfeeding experience will be like. You need to remember that your baby hasn’t read those books or taken those classes, and he doesn’t have a clue that he is supposed to behave like the “average’ baby. In reality, there is no such thing as an “average” baby. Since each mom and each baby is unique, each nursing experience will be different. None of my babies were ever average, that’s for sure. They were all the most beautiful, smart, talented, and and perfect babies in the world. Really, they were. At least until my grand babies arrived. :)
Often the mothers who have done the most intensive prenatal preparation are the ones who have problems adapting when things don’t go ‘right by the book’. In addition to joining online support groups, taking classes, or surfing Pinterest, it is important to have a support system in place in case you have questions after your baby is born (and you probably will), or if problems do develop. Find out about resources in your community. If medical problems develop, find out how to contact a Lactation Consultant in your area. Most of the time, your doctor doesn’t have the specialized training in lactation to provide the intensive help that an IBCLC (International Board Certified Lactation Consultant) can.
Here are some basic things you can do from the beginning to help get breastfeeding off to a good start:
- Breastfeed early. Put your baby to the breast as soon as possible after birth, while his sucking instincts are strongest. The bathing and measuring and temperature taking can wait. Babies are most alert during the first hour after birth, and soon settle into a sleepy stage than can last for hours or even days. Try to take advantage of this early alert period. Early feedings, before your milk comes in, give him a chance to practice while your nipple is soft and easy to grasp. Even if he doesn’t latch on and nurse during the first few minutes, he still gets a chance to nuzzle and smell and lick the nipple and areola, and that’s good practice for later on. Any sucking at all helps contract your uterus, reduces bleeding, and helps speed up delivery of the placenta.
- Nurse often. Room in with your baby, and learn to recognize his feeding cues (such as wriggling around, rapid eye movements, putting his hands in his mouth). Try not to wait until he is crying before you offer the breast. When he is crying and upset, he is less likely to be willing to settle down and nurse, and may respond by shutting down and falling asleep. Crying is a late feeding cue, so learn to recognize the early ones. Click here to see feeding cues.
- Newborns usually need to nurse 10-12 times or more in 24 hours. The more they nurse, the sooner your milk will come in, and the more milk your body will produce. Make sure that you offer the breast at least every two to three hours during the day, with no more than one four hour stretch during the night. Since newborns tend to be sleepy, you may have to wake him up for feedings. If you are separated from your baby after birth, or if he doesn’t nurse well, use a hospital or professional grade pump to stimulate and maintain your milk supply.
- Nurse for comfort as well as nourishment. Newborn babies have a strong need to suck, and the breast is nature’s original pacifier. Babies nurse for lots of reasons, and they are all valid. You really can’t overfeed a tiny newborn, so put him on the breast whenever he fusses. One of the greatest things about nursing is that you always have a built in pacifier – it works if he’s hungry, tired, lonely, sick, or scared. Don’t be afraid to use the breast as a pacifier – it works, makes your baby happier, builds your milk supply, and forces you to stop and rest.
- Plan to spend most of your time nursing in the early weeks. Try to get a shower and brush your teeth and remember to eat, but don’t take on anything much beyond that.
- If friends and family members want to help, let them take care of you while you take care of the baby. While everyone wants to hold the baby and give you a break, the most helpful thing they can do at this stage while you’re are resting and building your milk supply is to cook, clean, run errands, entertain older children, etc. There will be plenty of opportunities later on for them to play with the baby.

- Set up a ‘nursing station’ in the living room and the bedroom. Get all the supplies you will need together so you don’t have to move once you get settled: pillows, diapers, change of clothes, towel or cloth diaper for leaks or spit up, nursing pads, wipes, change of crib linens, bottle of water, laptop, cell, remote control, book to read, etc.
- Don’t limit the time he spends at the breast. Let him nurse as long as he seems interested. He needs to nurse long enough to get the high calorie hindmilk that comes later in the feeding, after the milk lets down. Especially in the early days of nursing, it may take several minutes for the let down reflex to ‘kick in’.
- Offer both breasts at a feeding. Nurse him at least ten to fifteen minutes on the first side, then burp and change him and offer the other breast. Next feeding, begin with the breast he nursed on last. Many babies will only take one breast at a feeding once your supply is well established, especially if you have a plentiful supply, but in the beginning, you need to stimulate both breasts.
- Avoid artificial nipples and supplemental feeding during the early weeks of nursing, if at all possible. While some babies switch back and forth from breast to bottle easily from the first day, some babies will become nipple confused if you introduce artificial nipples before they have mastered the art of breastfeeding.
- Don’t worry about your baby starving before your milk comes in. Colostrum, the yellow fluid that your breasts start producing during pregnancy, is the perfect first food for your baby and will meet all his nutritional needs for the first couple of days until your milk comes in. Here’s an interesting piece of trivia: in lower mammals, newborns die if they don’t receive the immunities from their mother’s colostrum. Ask someone who raises orphaned horses or puppies. The mother who refuses or is unable to nurse her newborn is dooming him, unless another lactating animal willing to accept the baby can be found ASAP. Thank goodness this isn’t true for humans! In the animal world, babies who are able to nurse for even a day or two have much a better chance of survival, due to the antibodies they receive to boost their immune systems.
- Colostrum is often called “baby’s first vaccine”. While colostrum isn’t quite as essential to human infants as it is to other mammals, it does provide important immune factors that newborn infants can’t receive anywhere else. It is easy to digest, and is full of antibodies and immune factors.
- During the first couple of days after your baby is born, he will take in only teaspoons (not ounces) of this precious fluid. His immature kidneys are not meant to handle large volumes of fluid at this time, and the colostrum has a laxative effect that clears the meconium (the black tarry first stool) out of his system. Excreting the meconium will help him avoid becoming jaundiced.
- Your baby is born with extra fluid in his tissues, and will pee and poop it out during the first day or so. Most babies will lose some weight in the first couple of days after birth. The average seven and a half pound baby will lose about 7% of his birth weight, or around eight ounces. This is normal, and he will quickly regain his weight in a few days once your milk comes in.
- Babies don’t need water, even when it is hot outside. Human milk contains plenty of water.
- Giving formula supplements at this early stage can cause all kinds of problems, including a decrease in your milk supply. Formula takes longer to digest than breast milk, so your baby stays full longer and is less likely to nurse as often as he needs to stimulate your supply. While many babies tolerate formula well, the younger your infant is when he is exposed to artificial milk, the greater the chance of allergies or digestive problems. The longer you wait to introduce formula (if you introduce it at all), the better.
- If supplements are medically indicated, (and they rarely are), it’s best to use alternate feeding methods rather than bottles. The article Introducing Bottles and Pacifiers to the Breastfed Baby has information on alternate feeding methods such as cup, syringe, tube, or finger feeding.
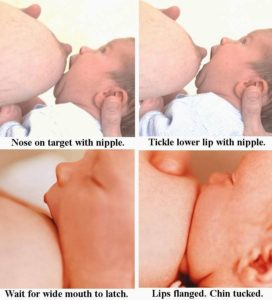 Make sure that your baby is latched on correctly and is nursing effectively. His mouth should be open wide, his lips flanged out, his tongue extended over his gum and under your nipple, and he should have not just the nipple but some or all of the areola (the dark area around the nipple) in his mouth as well. Try to see that he covers more of the areola with his lower with his lower lip than with his top lip – this way, he can get his lower jaw under the pockets of milk behind the areola and get the milk out more efficiently. He should be pulled in close with his chin and nose nearly touching the breast. His whole body should be facing yours, tummy to tummy, so that he doesn’t have to turn his head to nurse. (See photo of correct positioning). Here’s a video by Dr. Jack Newman that shows a baby latching on correctly. The article Sore Nipples contains additional information on how to make sure your baby is positioned and latched on correctly.
Make sure that your baby is latched on correctly and is nursing effectively. His mouth should be open wide, his lips flanged out, his tongue extended over his gum and under your nipple, and he should have not just the nipple but some or all of the areola (the dark area around the nipple) in his mouth as well. Try to see that he covers more of the areola with his lower with his lower lip than with his top lip – this way, he can get his lower jaw under the pockets of milk behind the areola and get the milk out more efficiently. He should be pulled in close with his chin and nose nearly touching the breast. His whole body should be facing yours, tummy to tummy, so that he doesn’t have to turn his head to nurse. (See photo of correct positioning). Here’s a video by Dr. Jack Newman that shows a baby latching on correctly. The article Sore Nipples contains additional information on how to make sure your baby is positioned and latched on correctly.- Learn signs of effective, nutritive nursing. Look for a long, drawing, rhythmic motion along his jaw-line, and a wiggling at his temple. You should be able to hear him swallowing after your milk comes in. Some babies will stay on the breast for long periods of time, but will ‘flutter suck’ ineffectively in their sleep, and won’t get the milk they need or supply you with the stimulation to produce more.
- Learn how to tell if your baby is getting enough milk. This is very important, since you can’t measure breast milk like you can formula. Keep track of urine and stool output, and check his weight early and often.
- For the first couple of days, your breasts will produce sticky yellow or gold colostrum. Your milk will ‘come in’ two to five days after birth, usually on the third day.
- Once your milk comes in, you will produce transitional milk – a mixture of colostrum and mature milk, which may be yellowish and creamy looking. During the next week or so, less and less colostrum is produced, and by the time your baby is two weeks old, mature milk has replaced the transitional milk and no more colostrum is produced.
- Get as much rest as you possibly can. During the first few couple of days after your baby arrives, both you and your baby are recovering from the stress of giving birth and being born. Babies tend to be sleepy during this time, and while you will be sleepy as well, it is often difficult to get much rest in the hospital. There is so much going on – blood pressure checks, temperature checks, visitors in and out, dealing with paperwork, getting the baby’s picture taken, having him circumcised, etc.
- BE PREPARED for days three and four. They are usually the roughest, and the time when most mothers are likely to give up and switch to formula. Many mothers tearfully call me on day three or four and say “But we did so well in the hospital! He nursed and slept, and everything was fine. Now he’s fussy, my nipples are sore, my breasts are hard, and I don’t know what to do!”
There are many reasons for this: the physical stress your body has been through (you often just don’t feed good – even with a natural childbirth with no complications, you are still physically drained, and you may be dealing with additional stresses like constipation, hemorrhoids, episiotomy stitches, or recovering from a c-section, and the hormonal upheavals, sleep deprivation, and overwhelming pressure of being the one person totally responsible for the nourishment of this new little person in your life. You also have the added pressure of worrying about the fact that your baby lost weight in the first couple of days after birth, even though this is normal.
While I understand the reasons for mothers being released from the hospital after twenty-four hours, I don’t think that many of the health professionals who decided to send you home so soon have done a good job of providing postpartum support, especially for breastfeeding. In most cases, you are home before your milk even comes in, and that’s why the support you have once you leave the hospital is so important.
It’s normal for babies to become agitated and fussy on the third or fourth day. Because he is born with extra fluid in his tissues, he really isn’t hungry during the first day or two, but nurses for comfort and because he loves to suck. Babies even suck their fingers while they’re in the womb.
Once babies pee and poop out the extra fluid, they experience hunger pangs for the first time, usually soon after mom and baby return home from the hospital and settle in at home.
Their little tummies rumble and growl, and they don’t like this new feeling one bit. They have no way of knowing that mom’s milk will come in soon, and if they go on the breast, they will get milk and feel full. They will soon figure it out, but it is a learning process. Be patient and hang in there.
- Don’t be surprised if your baby is jaundiced. Most infants are jaundiced to some degree. Nearly half of full-term infants, and four out of five preemies will become clinically jaundiced (skin and eyes have a visible yellowish tint). In the vast majority of cases, newborn jaundice is a normal process, which many researchers feel may even serve protective functions, such as guarding the infant from the effects of oxygen free radicals. It makes sense that something that occurs in the majority of babies so routinely may be part of nature’s plan for the human infant. Read the article “Jaundice In the Breastfed Baby” so that you won’t freak out if your doctor tells you that your precious newborn is jaundiced.
- Be prepared for growth spurts. These are periods of time when your baby wants to nurse constantly (or cluster feed), and never seems satisfied. These periods of rapid growth can be frustrating for both of you, but babies grow so quickly that sometimes they need to nurse more frequently in order to send your breasts the signals they need in order to produce more milk. Typically, growth spurts occur around 7-10 days, 3 weeks, 6 weeks, 3 months, and 6 months. Remember that they rarely last longer than a few days to a week. Once his frequent feedings build up your supply, he’ll go back to nursing on a more predictable schedule.
- Do whatever you have to do to survive the first two weeks. If you have to use slings, swings, bottles, pacifiers, formula, pain medicine, or drink a glass of wine, do it and don’t feel guilty about it. These things really won’t matter down the road, and sometimes they can make the difference between continuing to nurse or giving up in the early days. The most important thing is that you make sure your baby gets enough to eat while you lower your stress level and regain your strength.
- Even if you only nurse your baby for a few days or a couple of weeks, you are still providing him with important immune factors. (See Breastfeeding Benefits; How they Add Up). Very few mothers who make it through the first two weeks of nursing will give up at that point. That’s just when you are over the hump and things are starting to get easier. Most breastfeeding problems (sore nipples, engorgement, latch on problems, etc.) will be resolved after the first two weeks.
If you have been feeding every one to two hours around the clock, and your baby doesn’t go any longer stretches than that in twenty-four hours, consult a Lactation Consultant if this pattern continues longer than a few days. The baby who nurses ‘constantly’ for several hours, then sleeps for a four or five hour stretch, is probably still getting in his minimum of eight feedings in twenty-four hours, and is likely to be getting enough to eat. However, if he nurses ‘constantly’ around the clock with no long stretches between feedings and never seems satisfied, he may not be getting enough milk for a variety of reasons, and a consultation to discover the cause is indicated.
Know When to Ask for Help
- Your baby is not latching on well, or nursing just doesn’t “feel right’.
- Your breasts are engorged, or you are having breast or nipple pain, especially after the first couple of weeks. Breastfeeding is not supposed to hurt!
- Your baby is several days old and is not having 6-8 wet diapers and several bowel movements in each 24 hour period.
- Your baby is sleepy and hard to wake up for feedings. He is nursing less than 8 times in 24 hours.
- There are special circumstances such as jaundice, prematurity, low weight gain, cleft lip/palate, or neurological problems.
- You develop a breast infection (mastitis) or plugged ducts.
- You intend to return to work or school, or to be separated from your baby due to travel or hospitalization.
- You have any questions or problems related to breastfeeding.
Remember that the majority of breastfeeding problems can be solved if you are strongly committed to nursing your baby, and you receive advice and encouragement from a knowledgeable breastfeeding professional. Don’t ever be afraid to ask for help, but make sure that whoever you’re asking knows what they’re talking about. Sometimes the people who know the least about a topic are the first to give you advice about it, like people who’ve never had children giving you parenting advice.
La Leche League is a great resource for not only breastfeeding support, but also a wide range of information about parenting, nutrition, childbirth options, and more. La Leche League Leaders are moms who’ve nursed their own babies, and are trained to provide much needed support for pregnant or breastfeeding moms. Attending LLL meetings gives you a chance to meet other mothers who quickly become new friends, and provide a support system to help you get through the challenging early weeks of motherhood and breastfeeding.
La Leche League Leaders don’t give medical advice, but can provide you with information about which doctors in your area are ‘breastfeeding friendly’, and will know when to refer you to an IBCLC (International Board Certified Lactation Consultant) if you encounter difficult breastfeeding problems. Many times just talking to a la Leche League Leader, or to a friend who nursed her own baby, can reassure you that what you’re experiencing is normal and won’t last forever. Often, that may be all the support you need to hang in there until you’re over the bumps in the road that you may encounter in the early weeks of nursing.
Contact La Leche League to find out if there is a group in your area. You can also find a list of IBLCs in your area and how to contact them at http://kellymom.com/bf/concerns/bfhelp-find/.
(Edited October 2015)
Anne Smith, IBCLC
Breastfeeding Basics
*Please ‘Pay it Forward’!*
If you found any of the information in this article, helpful, please consider making a small donation to my favorite cause – Project Pets: Spay, Neuter, Love – all volunteer, non-profit organization that provides free spay and neuter services for homeless rescue dogs and cats…because every baby deserves a home, whether they have two legs or four! To find out how you can help, visit Project Pets on Facebook.
 Breastfeeding Basics
Breastfeeding Basics




